Lipedema (fat edema) — symptoms and treatment
Lipedema, also called fat edema, is a chronic, progressive condition that primarily affects women. It is a disorder in which fat tissue accumulates abnormally on the limbs, especially the legs, hips and sometimes the arms. It is important to know that this is not simple obesity — lipedema is a real disease that can significantly affect your quality of life.
Symptoms of lipedema and how to recognize it
If you have lipedema, you have probably already noticed that fat deposits appear symmetrically on both legs. The most typical pattern is fat accumulation from the hips down to the ankles, often in a "saddle" or "riding breeches" distribution. Interestingly, the feet usually remain slender, so a distinct "cuff" may form at the ankles. This is one of the main signs that distinguishes lipedema from simple obesity or lymphedema.
You may also experience nodules or lumps under the skin that feel like rice- or pea-sized structures. These areas are often tender to pressure and bruising can occur easily even with minor bumps.
Lipedema images and illustrations
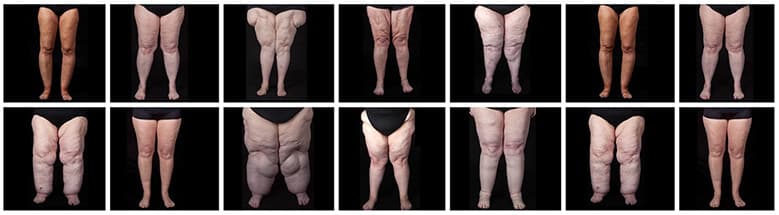
The appearance of lipedema can vary greatly. It can present differently in each affected person. The main features are shown in these images.
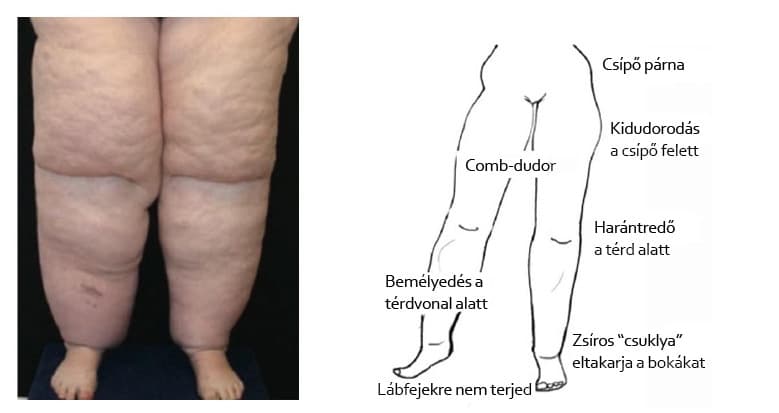
Symmetric changes and abnormal fat accumulation primarily appear on the lower limbs. Less commonly, the excess fat can also appear on the upper arms, most pronounced on the inner side of the elbow.
The fat surrounds the legs like riding breeches from the hips to the ankle line.
The foot remains slender! This helps distinguish it from general obesity, where fat pads are also visible. It also differentiates it from lymphedema, where the foot is usually the most affected and most swollen.
Characteristic findings include a bulge above the hip, a fat pad completely surrounding the kneecap, and a transverse skin fold forming below the knee.
The fat pad on the shin can hang over and cover the ankles.
Causes of lipedema
The exact cause of the disease is not yet fully understood, but researchers have identified several important factors. Hormonal changes play a key role — it is no coincidence that symptoms often begin or worsen during puberty, pregnancy or menopause. Genetic predisposition also plays a significant role, so if similar problems have occurred in your family, you should pay special attention to any symptoms.
Lipedema affects your everyday life!
Lipedema can significantly affect your life both physically and emotionally. Pain and a heavy sensation caused by the disease can limit your mobility and make you more easily fatigued. Many people also experience self-esteem issues because of the change in body shape. It is important to know that these feelings are natural and you are not alone.
Complications of lipedema
In more severe cases, the fat pads impair blood and lymph circulation and lymphedema can "add on," which significantly worsens the condition. Poor circulation also increases the fragility of blood vessels, so bruises can form on lipedematous areas even after minor trauma. In fat edema you often see blue-green discolorations on the limbs. Because of these tissue changes, the skin of the limbs becomes sensitive and can become painful even with light pressure.
A pathological condition, not "just" obesity!
Few physicians are familiar with fat edema. For a long time, affected people were treated simply as obese and beyond dietary advice, not much attention was paid.
Often years pass before someone finally makes the diagnosis: fat edema (lipedema).
From the patient's perspective, it is extremely important to recognize that it is the pathologically functioning fat tissue that causes the fat accumulation.
Lipedema diet
If you are affected, it is important to know that this is a disease that causes intensified fat accumulation even with a normal diet!
Although lipedematous fat tissue responds poorly to conventional diets, proper nutrition is still key.
The goal is not self-starvation or drastic weight loss, but following an anti-inflammatory diet.
Regular small meals and adequate fluid intake can also help manage symptoms.
Treatment of lipedema at home
Although you can live a full and active life with lipedema, it can cause a significant emotional burden regarding appearance. This may lead to low self-confidence, depression, social withdrawal, and even binge eating. Seek psychological help if you cannot cope alone!
For lipedema you should visit a lymphedema/compression therapy clinic. There, specialist nurses will give you lifestyle advice and teach you how to manage your condition at home.
Currently, lipedema is not a curable condition. However, you can stop its progression and reduce symptoms. This requires lifelong attention and daily, regular treatment. If you are affected, this is YOUR TASK! No one will do it for you, you will only receive guidance. In other words, arrange your life so that lipedema treatment becomes an integral part of it.
The cornerstones of treatment are compression garments, manual and machine-based compression therapy and regular physical activity.
With compression stockings
Wearing them effectively prevents symptom worsening and helps with prevention. They promote blood and lymph flow in the lymphatic system and thereby prevent fluid retention and the development of edema. The elastic garment moves the fluid in the tissues upward. Wearing compression garments halts or slows the progression of lipedema and its transformation into lipo-lymphedema.
The type and elasticity level of the compression garment best for you will be selected and prescribed by a specialist!
Compression alone may be sufficient in the early stages of fat edema, but it must be worn all day.
With manual therapy
Manual compression therapy (manual lymphatic drainage) is a special type of gentle massage that stimulates lymph flow and thereby reduces edema. It relieves uncomfortable tightness and possible pain. Combined with other treatments — wearing compression garments and machine-based compression therapy — it is most effective. Manual compression therapy requires special training, so choose a practitioner experienced in lymphatic drainage.
Lipedema and machine therapy
Machine-based compression therapy is performed in lipedema just as in lymphedema. Read my earlier article about this. A machine compression therapy unit requires a "boot" and/or "pant" cuff consisting of several airchambers.
The device sequentially inflates the cuffs' airchambers. With properly set pressure, the fat cell may be "opened" and fat can be "expressed" from it. The wave-like pressure propagation then "pushes" the fat out from the treated area.
Alongside machine treatments, continue to use compression garments and regularly include manual therapy, because together they are most effective.
Lipedema can be pressure-sensitive, so only buy a modern compression therapy unit whose cuff pressure is adjustable. Modern devices (for example the Power Q-2200 or the Power Q-1000 Premium) allow you to set the pressure so that it does not cause complaints but still improves symptoms.
In some cases fat edema "does not tolerate pressure." If compression treatments cause pain, do not perform them and stick to conservative measures.
Lipedema physiotherapy
Regular exercise is an important part of fat edema treatment and should preferably be done while wearing compression — i.e., exercise wearing your compression stockings!
As your muscles alternately contract, the stocking also expands and contracts elastically, thereby "pumping" the edema. Do lymphatic exercises at least three times a week for 60 minutes (you can learn them from a specialist and then perform them at home).
In addition, choose activities that do not overload the limb. Intense, vigorous running is not the right choice for you. Swimming, water aerobics, walking, leisurely cycling, and exercises on a vibration trainer are suitable.
Surgical treatment of lipedema
This section is an addition because many readers missed information about surgical options. In many places (primarily on plastic surgery clinic sites) liposuction is recommended for treating lipedema.
Older liposuction techniques were crude; they suctioned out fat with vacuum but in doing so often damaged lymphatic and blood vessels.
To avoid this, techniques have been developed and the newest liposuction methods are indeed less destructive. In lipedema, WAL (water-assisted), UAL (ultrasound-assisted), LAL (laser-assisted) and PAL (power-assisted/vibration) techniques are spreading.
What results can be expected from these procedures? A reputable clinic's website contains before-and-after photos. It is worth reviewing them.
There are several international organizations that bring together doctors treating lipedema. These medical groups regularly publish and update consensus treatment recommendations approved by their membership.
The American medical organization does not even mention liposuction on its website.
Others, such as the UK lipedema society, mention liposuction only as a treatment alternative in a separate category. They emphasize that there is no convincing data showing the procedure is risk-free in the long term. They recommend the method for the most severe stages that significantly limit quality of life, where it may improve quality of life despite possible long-term risks.
The biggest problem with liposuction is uncertainty. There are no data on whether there will be consequences in 10–15 years. Some medical groups argue that fat removal (in any form) is a drastic method that provides short-term benefits, but even the most modern techniques may damage lymphatic and blood vessels. Thus any form of liposuction could pose long-term risks by generating other problems (such as lymphatic and circulatory disturbances).
Current opinion is that a single liposuction session should remove at most 3 liters of fat. Therefore, in private care you must pay substantial sums; removing 20–30–50 liters would be extremely expensive. These surgeries are not funded by public health insurance.
On my blog I write about methods that are widely accessible, affordable, safe and helpful for many people. Liposuction is not among these. In my view, liposuction does not represent a realistic option for the majority of patients. It may help a few severely affected (or well-off) patients.
Lifestyle advice for everyday life
Numerous small changes in daily life can support treatment success. Avoid prolonged standing or sitting; change your position regularly. Slightly elevate your legs at night using an extra pillow. Buy comfortable, non-restrictive shoes and clothing.
Hot weather and hot baths can worsen symptoms, so pay special attention to compression therapy during summer and prefer lukewarm showers.
Psychological support and self-acceptance
Living with lipedema can be emotionally taxing. Do not be ashamed to seek professional help if you need support processing this. You can also join peer support groups to share experiences and support each other. Self-acceptance is a long process but an important part of successful treatment.
Summary — key to successful home management
Treating lipedema is a long-term process that requires persistence and patience. The key to success is regularity and a comprehensive approach — combining different treatment methods can yield the best results.
Remember that every patient is unique, so it may take time to find the most effective combination of treatments for you.
The most important thing is not to give up and believe that with proper treatment you can significantly improve your quality of life.
Keep in mind that although lipedema cannot be completely cured, it can be managed with appropriate treatment and lifestyle. With regular medical follow-up, home treatment and self-management are essential to keep symptoms under control and improve your quality of life.


