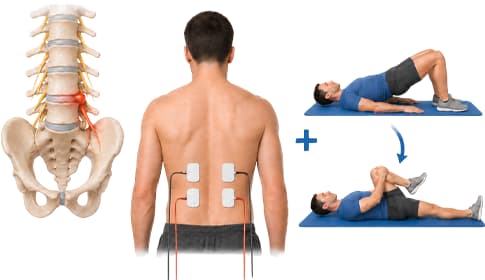
Why does it hurt and why doesn't it just go away?
Why does it hurt and why doesn't it just go away?
First, let's look at how and over what time frame the condition that ultimately causes a disc herniation develops.
The lumbar disc herniation (low back discus hernia) does not occur overnight. It develops over years, even decades, while the spinal support and back muscles gradually weaken and atrophy.
Sedentary lifestyle, asymmetric loading, long periods of standing work, or prolonged overload from hard physical labor: they all lead to the same outcome. The spine-stabilizing muscles weaken and lose their function, and increasingly more load is placed on the intervertebral discs. The ever-growing pressure—without the supporting strength of the muscles—the disc cannot bear on its own anymore – the moment comes when it ruptures, much like a jam-filled doughnut when you press on it.
 The essence of disc herniation
The essence of disc herniation
Disc herniation is primarily due to insufficiency of the protective and stabilizing muscular system surrounding the vertebrae (in plain words: weakness of the supporting muscles). If the muscles regain strength, the spine stabilizes, the load on the discs decreases, and symptoms can be alleviated.
The logic of disc herniation rehabilitation follows from this: if the problem is caused by muscle weakness, then rebuilding the muscular system is the foundation of the solution.
It is important to know that only muscle contraction can strengthen a muscle. Muscles cannot be strengthened with medications, injections, or even surgery. Rest and protection certainly won't strengthen them either—they only weaken the muscles further.
The most effective way to strengthen muscles is exercise—this is how symptoms can be prevented.
If a herniation has already developed, physiotherapy can help—but by then there can already be a serious obstacle: pain. When the herniation is active, movements and exercises are painful. Because of this, the patient performs the exercises less often and with lower intensity. The protected (non-mobilized) muscle not only fails to strengthen but weakens further, and the pain persists. The circle closes.
This negative cycle can be interrupted with the help of electrical muscle stimulation. We generally do not recommend it instead of exercise, but to complement and increase the effectiveness of physiotherapy.
There are some cases where the pain is so severe that even the gentlest exercises are not possible. In these situations muscle stimulation is practically the only way to reduce pain enough to allow spinal physiotherapy to be performed at all.
 How can EMS help in spinal rehabilitation?
How can EMS help in spinal rehabilitation?
The electrical muscle stimulation (EMS), also called neuromuscular electrical stimulation (NMES), works by delivering electrical impulses through the skin to the muscles, which respond with contractions—just like voluntary movements required to produce a muscular action.
The result is visible and tangible: muscle contraction.
It is important to distinguish between two different mechanisms of action used in the treatment of spinal disorders:
The primary goal of EMS/NMES in disc herniation rehabilitation is to evoke muscle contraction—especially of the deep stabilizing muscles that are barely activated voluntarily in chronic pain conditions.
Research shows that with electrodes placed alongside the L4–L5 level, NMES can simultaneously activate the multifidus and the deep abdominal stabilizing layer—so the device works both the back and the abdomen at the same time.1,3
This effect is particularly important when pain prevents the patient from voluntarily contracting these muscles with sufficient force—the EMS essentially “takes over control” and performs the muscular work.
TENS (transcutaneous electrical nerve stimulation) works by a different mechanism: it stimulates sensory nerves rather than the muscle and thus inhibits the transmission of pain signals to the brain (gate theory). The result: pain reduction that can persist during the treatment and for a short time afterward.2
However, the scientific literature clearly indicates: TENS alone is not sufficient in disc herniation rehabilitation. It reduces pain but does not strengthen muscle, improve functional abilities, or activate deep stabilizers. Pain relief alone does not lead to lasting improvement.
The real role of TENS is as a preparation for exercise, so that with reduced pain levels physiotherapy can be performed more intensively and for longer durations.
Research indicates that the most effective approach is the combined application of NMES and movement therapy (motor control exercise, MCE). A 2021 randomized trial found that the combined NMES+MCE group showed significantly greater improvement in multifidus activation than the group doing exercise alone.4
The logic: NMES “warms up” and pre-activates the deep spinal muscles, which then can participate more effectively in exercise tasks. This is a form of neurological priming—the device awakens motor units that the brain's controlling mechanisms had shut down due to the herniation.
In summary: NMES or EMS + active stabilizing exercise = the most effective home rehabilitation combination when pain, post-surgical status, or limited mobility prevents purely voluntary training.
Why is physiotherapy alone not always sufficient?
Many people are puzzled: they completed the “prescribed” 10–15 physiotherapy sessions and still saw no result. There are several identifiable reasons for this.
| Common physiotherapy problems | Why does it happen? | How EMS helps |
|---|---|---|
| Too short, too infrequent | Daily 15-minute exercise is not sufficient for lasting muscle building. Athletes train for years—the chronic atrophy does not heal in 2 weeks. | EMS can be performed multiple times daily, complements exercises, and fills the muscle-work deficit. |
| Pain interferes | If the exercises are painful, the patient does them less and with less effort. The muscle does not receive sufficient stimulus. | EMS produces muscle contraction without pain or at a reduced pain level. TENS pre-treatment can mitigate pain. |
| Deep muscles do not activate | Deep muscles are neurologically inhibited in chronic pain—no matter how much the patient exercises, these muscles do not work properly. | Stimulation targets the muscles directly, bypassing central nervous system limitations.1,3 |
| Lack of motivation and persistence | Maintaining regular, intensive exercise for 6–8 months is difficult from self-motivation alone, especially when results are slow to appear. | EMS is easier to integrate into daily routine, can be used while lying down, and the perceptible muscle tension signals that it is "working." |
 EMS does not replace exercise in the long run
EMS does not replace exercise in the long run
Electrical muscle stimulation is an effective aid, but do not rely on it exclusively! Initially, EMS plays an important role. As soon as pain decreases enough to allow exercise, gradually increase exercise and reduce EMS. Over time, EMS becomes a supplement.
For which spinal problems and when is it worth using EMS?
Disc herniation is not the same for everyone. The following helps you navigate when and how EMS can be incorporated into rehabilitation for different conditions.
In classic low back disc herniation, EMS can primarily assist the work of spinal stabilizing muscles (multifidus, paraspinalis, transversus abdominis). It can be particularly useful when pain prevents exercises from being performed at the necessary intensity and frequency. With a 4-channel arrangement, the back and abdominal muscles can be stimulated simultaneously.1
Disc degeneration and spinal osteophytes (spondylosis) are also associated with weakening of the muscular system. EMS can help here as well via muscle stimulation: active musculature provides better circulation to tissues around the disc and reduces static load on the spine.5
In sciatica, a clinical study examining the effects of electrostimulation (Wang et al., 2018) found that electrostimulation significantly reduced pain and improved clinical symptoms in sciatica caused by disc herniation.2 Important: in cases of sciatica, medical consultation is always necessary to determine the treatment protocol.
Many people return home from rehab knowing what they should do, but stabilizing exercises are harder to do at home: there is no physiotherapist, no supervision, and motivation wanes sooner. A home EMS device can help continue the muscle work, complementing the stabilizing exercises done at home.
 Home EMS devices for spinal rehabilitation
Home EMS devices for spinal rehabilitation
For lumbar disc herniation, a home EMS treatment requires at least a 4-channel device so that the back and abdominal muscles can be treated simultaneously. I present the devices below because their programs are suitable even for clinical rehabilitation needs.
Globus Genesy 300 Pro
Both are semi-professional devices with a wide range of programs. Their detailed NMES and muscle-strengthening protocols make them suitable for longer, structured rehabilitation treatments.
Which program should I use?
For spinal rehabilitation you should primarily use the device's EMS (muscle-strengthening) programs to activate and strengthen the muscles. A TENS program can help reduce pain, especially before or after exercise. Specific parameters and electrode placement can be found in the detailed program plan.
 Before you start home EMS treatment
Before you start home EMS treatment
EMS treatment is generally safe, but there are situations in which medical consultation is necessary, or in which the treatment cannot be performed.
When NOT to apply EMS to the lower back?
- Active, acute inflammatory phase – if the herniation is active and accompanied by strong radiating pain, pain relief is required first. In such cases, EMS aimed at strong contractions and muscle strengthening is not yet recommended.
- Older implanted electrical devices (e.g., pacemaker, spinal cord stimulator) may interfere with the treatment. Always consult your physician.
- Pregnancy – abdominal and lower back stimulation is contraindicated in pregnant women.
- Cancer in the treatment area – electrostimulation must not be used near malignant tumors.
- Fresh surgical area – avoid electrostimulation over the surgical area until wound healing is complete (generally at least 2–3 weeks).
- Skin disease, injury, or loss of sensation in the treatment area – electrodes cannot be placed on damaged skin; with loss of sensation the current intensity cannot be controlled properly.
Consult your treating physician
In case of disc herniation it is always advisable to discuss home EMS treatment with your treating physician or physiotherapist, especially if neurological symptoms (numbness, weakness) are present. EMS is an adjunctive therapy—it does not replace comprehensive medical care.
 Scientific background
Scientific background
Below I summarize studies that form the scientific basis for the application of EMS/NMES in spinal rehabilitation.
NMES activates deep spinal stabilizers (Kim et al., 2016)
In a thirty-patient sample, three different NMES application protocols were investigated: abdominal-only, posterior-only, and simultaneous abdominal+posterior stimulation. Results showed that all three protocols significantly increased the thickness of the examined stabilizing muscles (multifidus, transversus abdominis, internal oblique) compared to resting state. The best result was achieved with simultaneous abdominal and posterior electrode placement.3
EMS + exercise is more effective than exercise alone (Songjaroen et al., 2021)
A randomized trial on 25 healthy and 35 individuals with motor control impairments found that the NMES+MCE (motor control exercise) combination produced significantly better multifidus activation than exercise alone. The researchers suggest that NMES's pre-activation effect prepares the deep muscles for exercise tasks.4
Electrostimulation reduces pain in sciatica (Wang et al., 2018)
One hundred patients diagnosed with sciatica due to disc herniation were randomized into control and experimental groups. The electrostimulation treatment used in the experimental group produced significantly lower pain scores (PRI, PPI, and VAS) four weeks after starting therapy compared to standard traction treatment.2
TENS alone is not sufficient (França et al., 2019)
A randomized study of 40 patients with lumbar disc herniation compared motor control training (MCT) and TENS treatment. Result: MCT proved more effective in reducing pain, improving functional ability, and activating the transversus abdominis. TENS alone was effective only for pain relief—not for muscle function or disability.5
Systematic review: EMS improves trunk muscle endurance (2023)
A 2023 systematic review and meta-analysis evaluated ten studies on the effect of lumbar electrotherapy (EMS, NMES, TENS, IFC) on spinal muscle morphology and function. Based on limited evidence, both EMS alone and EMS+exercise combinations were more effective than passive controls in improving trunk muscle endurance. NMES also outperformed passive control in terms of muscle strength.6
How to incorporate EMS into your spinal rehabilitation?
The key to effectiveness is consistency and gradual progression. Here are some concrete basic principles to follow.
Principles of EMS treatment in disc herniation
Start with low intensity: during the first few days only go slightly above the sensory threshold—you feel the electrical impulse, but strong muscle twitching is not yet necessary. Gradually increase intensity until visible muscle contraction appears.
Two regions, four channels: if possible, treat both sides of the lower back and the lower abdomen (transversus abdominis) simultaneously. Research indicates that this combined arrangement yields the best results.3
Treatment daily, not once or twice a week: the effect is cumulative. One, preferably two daily sessions of 20–30 minutes each are realistically achievable at home and represent the minimum stimulus required for lasting muscle building.
EMS before or after exercise: EMS can be used both before and after physiotherapy. Before exercise the "Warm-up" program pre-activates muscles. After exercise the "Active recovery" program rests the worked muscle and reduces pain.
Patience! At least 3–4 months: just as muscle weakness did not develop in one or two weeks, rebuilding the muscular system also takes time. Those who follow this combined (EMS + exercise) program regularly for at least 3–4 months can expect meaningful change.
 Frequently asked questions
Frequently asked questions
EMS and combined movement therapy do not promise to avoid surgery—only your physician can judge that based on your individual condition, imaging results, and neurological symptoms. What research supports is that conservative treatment (which may include EMS) can often make surgery unnecessary, especially if applied early and consistently. However, if neurological deficit symptoms (leg muscle weakness, sensory loss, incontinence) are present, surgery cannot be delayed.
The two serve different goals and ideally are used together. TENS reduces pain via the nervous system—fast, temporary effect. EMS works the muscle and contributes to long-term rebuilding of musculature. In disc herniation rehabilitation the muscle-strengthening EMS program is more important—TENS helps reduce pain enough to allow EMS and exercise to be performed. The best choice is a device that contains both program types.
Research-based optimal placement: two electrodes on either side of the lumbar spine (at the L4–L5 level, approximately 2–3 cm from the spinous processes), and two electrodes on the lower abdomen (below the navel, over the transversus abdominis). This four-electrode arrangement activates back and abdominal stabilizers simultaneously. Detailed electrode placement guidance can be found in the lumbar EMS program plan article.
With realistic expectations: pain reduction may appear within a few weeks if you use EMS and exercise regularly. Meaningful muscle rebuilding and lasting improvement require at least 6–8 months of regular, daily work. This is not a limitation of the device—exercise requires the same amount of time. Muscle biology regenerates and strengthens at this pace.
Research on deep abdominal stabilizers found that 50 Hz NMES produced greater increases in muscle thickness than 20 or 80 Hz. For multifidus activation a frequency between 30–50 Hz is typically recommended, while pain-relieving TENS programs usually use ranges of 80–150 Hz. Most home EMS devices provide these as preset programs.
 Summary – Quick overview
Summary – Quick overview
Sources
- Yun SJ, Park HJ, Cha YJ, Oh JW (2014). Activations of deep lumbar stabilizing muscles by transcutaneous neuromuscular electrical stimulation of lumbar paraspinal regions. Annals of Rehabilitation Medicine. PubMed: 25229029
- Wang L, Fan W, Yu C, Lang M, Sun G (2018). Clinical effects of electrical stimulation therapy on lumbar disc herniation-induced sciatica and its influence on peripheral ROS level. Journal of Musculoskeletal and Neuronal Interactions. PubMed: 30179218
- Kim SY, Kim JH, Jung GS, Baek SO, Jones R, Ahn SH (2016). The effects of transcutaneous neuromuscular electrical stimulation on the activation of deep lumbar stabilizing muscles of patients with lumbar degenerative kyphosis. Journal of Physical Therapy Science. PMC4792980
- Songjaroen S, Sungnak P, Piriyaprasarth P, Wang HK, Laskin JJ, Wattananon P (2021). Combined neuromuscular electrical stimulation with motor control exercise can improve lumbar multifidus activation in individuals with recurrent low back pain. Scientific Reports. PubMed: 34285318
- França FJR, Callegari B, Ramos LAV, Burke TN, Magalhães MO, Comachio J, Marques AP (2019). Motor Control Training Compared With Transcutaneous Electrical Nerve Stimulation in Patients With Disc Herniation With Associated Radiculopathy. American Journal of Physical Medicine and Rehabilitation. PubMed: 30247159
- Moutzouri M, Falla D, Moore A, Rushton A (2023). The Effect of Transcutaneous Electrotherapy on Lumbar Range of Motion and Paraspinal Muscle Characteristics in Chronic Low Back Pain Patients: A Systematic Review and Meta-Analysis. Journal of Clinical Medicine. MDPI: 10.3390/jcm12144680