 Why is exercise important in lipedema?
Why is exercise important in lipedema?
One of the most important yet most underestimated elements of lipedema management is regular movement. Clinical trials convey a clear message: pneumatic compression (mechanical lymphatic massage) or a compression garment alone does not produce as lasting results as a combined treatment supplemented with exercise. The muscle-pump function (the calf, thigh and upper-arm muscles) has been shown to improve venous return and lymphatic flow — this is especially helpful in patients with lipedema, where increased tissue mass already makes fluid flow more difficult.
However, exercise therapy for lipedema does NOT mean a classic, intensive “training plan.” The key is: exercise while wearing a compression garment, at low-to-moderate intensity, and preferably daily for shorter periods rather than a few long sessions each week. The goal is not weight loss or muscle hypertrophy — but to preserve the muscle pump, maintain mobility, and reduce chronic inflammation.
 Key idea
Key idea
The 3 basic rules of exercise for lipedema: in a compression garment, at low-to-moderate intensity, and regularly, daily. This approach can help relieve symptoms, slow stage progression, and improve quality of life.
5 basic rules for lipedema exercise
Before starting any exercise protocol, it is worth understanding and following these 5 basic rules.
- Exercise in a compression garment. Class II compression stockings/sleeves (23–32 mmHg) support lipedematous tissues, reduce joint load, and optimize venous return. Exercising without compression in lipedema can have the opposite effect — increased tissue pumping may exacerbate swelling.
- Start at low intensity. If you are just beginning, 15–20 minutes of walking or swimming 2–3 times a week is sufficient. You can gradually increase duration and frequency. A "do-everything-at-once" approach leads to rapid fatigue and giving up.
- Cool or lukewarm environment. Hot baths, saunas and overly warm gym environments increase swelling due to vasodilation. Exercise in cool air (18–22 °C), and for water activities aim for water temperatures below 28 °C.
- Avoid high-impact activities. Running on hard surfaces, jump rope, trampoline work, and jump-type HIIT exercises can damage joints in lipedema (especially the knee). Replace them with low-impact alternatives: swimming, cycling, elliptical trainer, uphill walking.
- Hydrate and rest. Increased fluid intake during and after exercise (to replace losses from sweating) and recovery days (1–2 rest days per week) are integral parts of the protocol.
Swimming and water exercise — the golden rule for most with lipedema
Water exercise is absolutely the "gold standard" among lipedema-oriented exercise forms. Three factors make it ideal:
- Hydrostatic pressure: water provides natural, circumferential compression to the limb, which supports venous and lymphatic return.
- Buoyancy: due to water buoyancy, joint loading is substantially lower than on land. It is safe even with knee and hip complaints.
- Cooling effect: the water temperature (usually 26–28 °C) cools the tissues, reducing vasodilatory responses.
Recommended swimming styles for lipedema:
- Backstroke: the gentlest, works the back and thigh muscles evenly.
- Breaststroke: strengthens calf and hip muscles but requires attention to the knee joint.
- Water walking: when the water reaches shoulder level — a simple, very gentle alternative suitable even for non-swimmers.
- Aqua fitness: group classes that incorporate functional exercises in the water. Aqua classes specifically organized for people with lipedema are available in several Hungarian pools.
Recommended weekly duration: 2–3 sessions × 30–45 minutes. If you have access to a pool, water exercise should form the backbone of your exercise protocol.
Walking — the fundamental daily activity
Walking is the most accessible yet effective form of exercise. It has particular value in lipedema because the muscle-pump function in the thigh and calf muscles is optimal. Clinical practice recommends 30 minutes daily at a moderate pace (about 4–5 km/h) while wearing compression stockings. More is not contraindicated!
Tips for effective lipedema walking:
- Periodic "intensity spikes": during a 30-minute walk, increase the pace 3–4 times for 1–2 minutes. This enhances the muscle-pump effect without causing the impact of running.
- Uneven terrain: hills, slopes, stairs — these work the calf and thigh muscles more than flat walking. You can moderately include hikes.
- Avoid hard asphalt if possible: in autumn and winter this is not always avoidable, but if you can choose, parks, forest paths and grassy trails are gentler on the joints.
- Proper shoes: sports shoes with good soles and shock absorption are essential. Classic city shoes are not ideal for daily walks of 30+ minutes.
- Persistent compression: wear the compression garment during the entire walk; after the walk do not remove it immediately — allow volume stabilization to occur.
If you are currently not active, start with 3 sessions per week × 15 minutes, and gradually increase to 30 minutes daily over 2–3 weeks. A step counter (phone app or smartwatch) can help track trends — long-term, 6,000–8,000 steps daily is an ideal training target for lipedema.
Cycling — a low-impact alternative
Cycling (at home or outdoors) is one of the best exercise choices for lipedema because it is specifically low-impact while actively working the thigh and calf muscles. The home version (exercise bike, elliptical trainer) is particularly convenient as it is not affected by weather.
Home cycling protocol for lipedema:
- Duration: 20–30 minutes at moderate resistance.
- Cadence: 60–80 revolutions per minute — rhythmical pedaling is more important than speed.
- Resistance: moderate — not so high that you cannot maintain 60–80 rpm.
- Posture: keep a straight back, avoid leaning forward. The classic "spinning" forward-leaning posture is not ideal for the knee joint.
- Weekly frequency: 3–4 sessions (or alternated with other exercise forms).
Outdoor cycling: flat or gently rolling terrain is ideal. Mountain biking (off-road trails with jumps) is not recommended for lipedema — joint loading is too high. Longer flat rides, however, are particularly gentle and enjoyable.
Functional strengthening exercises
Maintaining muscle mass is particularly important in lipedema: muscle supports venous and lymphatic return, and higher muscle mass provides a better metabolic state. Classic heavy-weight, fast-repetition strength training is not optimal — functional, controlled exercises with moderate load are recommended instead.
Lipedema-friendly strengthening exercises (2–3 times weekly, 20–30 minutes):
- Bodyweight exercises: wall-supported squats, planks, push-offs using a chair. Bodyweight is sufficient.
- Pilates: highly recommended. Slow, controlled movements focusing on core stabilization and deep musculature. Look for Pilates classes suitable for people with lipedema.
- Yoga: but NOT "strong" styles (vinyasa, ashtanga, hot yoga). "Hatha" or "restorative" yoga is ideal. Many poses improve venous and lymphatic circulation (legs-up-the-wall, inverted poses).
- MovesBand exercises: arm and leg strengthening with an elastic resistance band. Gentle, and can replace weighted training.
- Water weight exercises: in the pool with water dumbbells — combine the benefits of water exercise with controlled strengthening.
To avoid: CrossFit (especially jumping and Olympic-lift elements), HIIT, Tabata-style intervals, heavy weight training (squats with 100+ kg), heavy deadlifts. These exercises increase loading on knee and hip joints in lipedema.
Lymph-focused movement protocol (lymph-yoga)
"Lymph-yoga" or "lymphatic movement" is a specialized exercise system combining principles of classical yoga and manual lymphatic drainage (MLD). The exercises are based on slow, rhythmic, gentle movements aimed at supporting unobstructed flow through lymphatic pathways. This is useful in lipedema and lymphedema alike.
5 lipedema-oriented lymph exercises (daily routine, 10–15 minutes):
- Supine leg pump: lie on your back with legs elevated, soles toward the ceiling. Slowly perform rhythmic leg lifts for 1 minute.

- Legs-up-the-wall: lie on your back with legs vertical against the wall. Hold for 5 minutes. A classic yoga pose that aids venous return.

- Ankle circles in both directions: sitting or lying down, rotate the ankles slowly in circular motions for 30 seconds one way and 30 seconds the other.

- Thigh extensor stretch: sitting with one leg extended, place your hands above the knee and slowly lean forward. Hold 30 seconds, then switch legs.

- Deep abdominal breathing: lie on your back with your hand on your abdomen. Breathe in slowly, expanding the belly, then exhale fully. 5 minutes. Diaphragmatic movement stimulates clearance of the abdominal lymph region.
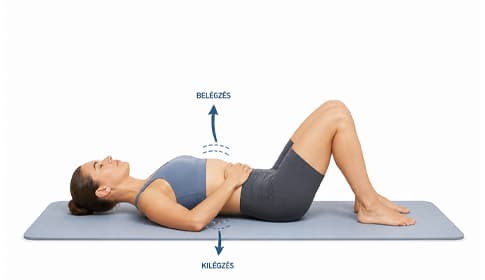
Perform these exercises after waking up or before bedtime. They are not tiring but support fluid flow and venous-lymphatic return. Ten to fifteen minutes daily is sufficient.
One-week sample protocol (home, beginner level)
The sample week below is intended for a beginner with lipedema who is starting an exercise routine. Follow this in the first weeks, then gradually increase duration and frequency.
| Day | Exercise | Duration |
|---|---|---|
| Monday | Morning: 10 minutes of lymph exercises. Evening: 30 minutes walking in compression stockings. | 40 minutes |
| Tuesday | Swimming or aqua fitness (if a pool is available) or 30 minutes of home cycling. | 30–45 minutes |
| Wednesday | Morning: 10 minutes of lymph exercises. Evening: 20 minutes of Pilates or hatha yoga. | 30 minutes |
| Thursday | 30 minutes walking + 10 minutes MovesBand exercises for arms and legs. | 40 minutes |
| Friday | Swimming or aqua fitness or 30 minutes of home cycling. | 30–45 minutes |
| Saturday | Longer walk, hike (60+ minutes) on gentle terrain. | 60+ minutes |
| Sunday | Rest day. Morning: 10 minutes of lymph exercises and gentle stretching yoga. | 20 minutes |
This weekly routine totals about 4 hours of activity, which falls within clinical recommendations (150 minutes of moderate-intensity exercise per week). Regularity is more important than a single long workout.
What to avoid? Harmful exercise forms in lipedema
Some popular exercise forms are specifically harmful in lipedema. The following should be minimized or completely avoided:
- HIIT (high-intensity interval training): jump-type elements place severe load on the knees and hips in lipedema. The strong heart-rate fluctuations also increase venous circulation stress.
- Running on hard surfaces without compression: asphalt running and the impact of running can cause early knee cartilage wear. If you want to run, do so in compression stockings, on gentle surfaces (park, forest path), and only for short distances.
- Long sauna or steam sessions: high temperatures cause vasodilation and can worsen swelling. Short exposure (max. 5–10 minutes) followed by a cool shower is acceptable.
- Prolonged static standing or sitting: all-day immobility worsens venous return. If you have a desk job, move for at least 5 minutes each hour (walk the corridor, do ankle circles while seated).
- Very heavy weight training: squats with 100+ kg, deadlifts or extremely heavy bench presses are not recommended. Functional, moderate-load strengthening is the appropriate direction.
- CrossFit, military fitness: combined fast, high-intensity exercises are unsuitable for lipedema. Functional strengthening and water exercise are alternatives.
If you notice increasing swelling, pain, or skin discoloration during any exercise, stop and observe the limb. Worsening symptoms indicate excessive load — reduce intensity or duration.
When should you consult a physiotherapist or physiotherapy specialist?
Home exercise protocols can work well independently, but in certain situations professional involvement is strongly recommended:
- Severe (stage 3–4) lipedema: where mobility is already significantly reduced and standard home protocols are too difficult. A physiotherapist experienced with lipedema can create an individually tailored program.
- Practitioners with lymphatic therapy experience: physiotherapists trained in MLD (manual lymphatic drainage) can also competently address exercise therapy aspects.
- Knee or hip joint complaints: if gonarthrosis has begun or another mechanical problem has appeared, orthopedic consultation and functional physiotherapy are necessary.
- Postoperative period: after liposuction or lipedema-oriented surgical procedures, restarting exercise should be supervised by a professional. Details in the Lymph reconstruction surgery guide.
- Water exercise group: aqua classes specifically organized for people with lipedema are available in several Hungarian pools — it is worth finding such a group in your area.
Professional support is especially useful in the first 1–3 months when you are still learning appropriate exercise forms and posture. Group sessions (lipedema exercise classes, aqua groups) also provide social and psychological support.
 Clinical evidence in the field of lipedema exercise
Clinical evidence in the field of lipedema exercise
The clinical evidence base linking lipedema and exercise therapy is moderate but growing. The key message of the studies below: a multimodal approach (exercise + compression + IPC) produces better results than isolated interventions.
Atan and Bahar-Özdemir (2020) – CDT vs IPC vs exercise RCT, severe lipedema
In 33 women with severe (stage 3) lipedema, the combination of complete decongestive therapy (CDT) + exercise produced the greatest reduction in limb volume, pain and physical function. IPC + exercise also yielded significantly better results than exercise alone. The study clearly shows that exercise therapy by itself is not sufficient — combined with compression and pneumatic compression it significantly strengthens the treatment package.1
Esmer and Schingale (2024) – CDT + IPC + lifestyle in lipedema
Twenty-two women with lipedema showed reductions in both intracellular and extracellular fluid volumes after a one-month CDT + IPC + lifestyle protocol. Regular exercise was part of the protocol. The authors suggest the combined therapy may slow stage progression, and exercise is an important component of the package.2
Wright et al. (2022) – PCD + conservative care (with exercise elements)
In the pneumatic compression device + conservative care (PCD+CC) group, the conservative component included regular exercise and wearing compression garments. The combined group achieved significantly better results than conservative care alone (compression + exercise without IPC) — indirectly supporting that the three elements (compression + exercise + IPC) work best together.3
The clinical message is clear: exercise is an indispensable pillar of lipedema treatment, but it is not sufficient on its own. The most effective approach combines a compression garment + IPC + exercise + lifestyle elements, coordinated with your treating physician or lymph therapist.
Deeper guides in the cluster
Related guides for the full lipedema treatment package:
- Lipedema (fat edema) symptoms and treatment – pillar guide
- Lipedema stages 1–4 – stage-level guide
- Lipedema or lymphedema? – differential diagnosis
- Lipedema diet – anti-inflammatory nutrition
- Lipedema-fat edema category – stage-level product recommendations
- Lymphatic massage device – multi-indication hub – device selection
- Lymphatic massage device – what it is for, how to choose? – technical guide
- Lymphatic drainage – manual and mechanical lymphatic massage – physical treatment
- Compression therapy for athletes – exercise and recovery context
- Lymph reconstruction surgery – surgical options
 What to consider before starting lipedema exercise?
What to consider before starting lipedema exercise?
Exercise is generally safe in lipedema, but in some conditions medical consultation is definitely required before starting.
Warning factors
- Acute deep vein thrombosis or suspected DVT – treatment should be paused and immediate medical consultation is necessary.
- Severe heart failure, uncontrolled high blood pressure – exercise protocols only under medical supervision and individualized.
- Active skin infection (erysipelas, cellulitis) in the treated area – exercise should be paused until the infection has healed.
- Fresh postoperative period (e.g. liposuction) – not recommended until wound healing and approval from the treating physician.
- Severe joint problems (advanced gonarthrosis, post-hip surgery phase) – exercise protocol tailored with an orthopedist and physiotherapist.
- Severe asthma or COPD – pulmonologist consultation is required to define the exercise protocol.
 Important information
Important information
Exercise therapy is an important element of multimodal lipedema treatment, but it does not replace medical or physiotherapy care. For new complaints, increasing swelling, pain or skin changes, consult your treating physician or physiotherapist. When starting a new exercise program always begin at low intensity and monitor symptoms.
 Frequently asked questions
Frequently asked questions
Initial signs (less heavy-leg sensation, more energy, easier mobility) are typically noticeable within 2–4 weeks. More significant changes (reduced pain, size stabilization) develop over 2–6 months. Regularity is key — 4–5 sessions per week of moderate exercise is worth more than 1–2 long workouts weekly.
Generally not recommended. A compression garment supports lipedematous tissues during exercise and optimizes venous-lymphatic return. Exercising without compression can increase swelling and local tissue pressure. Exceptions: water exercise (hydrostatic pressure of the water substitutes for compression) and slow lymph-focused exercises performed supine. In other cases, exercise with a compression garment is advised.
Transient mild swelling after exercise (1–2 hours) is normal. If swelling is persistent (more than 4–6 hours) or worsens: 1) reduce intensity or duration at the next session, 2) check that the compression garment size and compression class are appropriate, 3) use a pneumatic compression device after exercise as a maintenance protocol. If the problem persists, consult your treating physician or lymph therapist.
Fatigue and pain in lipedema are real symptoms, not a matter of willpower. Some practical tips: 1) Start small — three 10-minute sessions per week is plenty to begin. 2) Choose activities you enjoy — aqua classes are often more pleasant than home exercises. 3) Join a community — group classes or lipedema exercise sessions provide regularity and social support. 4) Keep a log of exercise and symptoms — seeing gradual improvement makes it easier to maintain motivation.
Yes. Patients with lipedema are prone to overtraining because they hope more activity will bring rapid improvement — this is counterproductive. Signs include persistent (24+ hours) increased swelling, worsening pain, marked exhaustion, sleep disturbance, and recurrent skin irritation. If you experience these, reduce intensity and duration and include more rest days. Motto: "slow and regular" serves better than "fast and intense."
Generally yes, but the exercise protocol should be developed together with your obstetrician and your lipedema specialist. Water exercise and walking in compression stockings are usually safe. Higher-intensity activities (HIIT, advanced Pilates, heavy weight training) should be avoided. In the last trimester, exercise may be reduced and the focus shifted to gentle lymph exercises (legs-up-the-wall, diaphragmatic breathing).
 Summary – Lipedema physiotherapy in brief
Summary – Lipedema physiotherapy in brief
Sources
- Atan T, Bahar-Özdemir Y (2020). The Effects of Complete Decongestive Therapy or Intermittent Pneumatic Compression Therapy or Exercise Only in the Treatment of Severe Lipedema: A Randomized Controlled Trial. Lymphatic Research and Biology. DOI: 10.1089/lrb.2020.0019
- Esmer M, Schingale FJ (2024). Can Physical Therapy Techniques Slow Down the Progression of Lipedema?. Lymphatic Research and Biology. DOI: 10.1089/lrb.2024.0065
- Wright T, Scarfino CD, O'Malley EM (2022). Effect of pneumatic compression device and stocking use on symptoms and quality of life in women with lipedema: A proof-in-principle randomized trial. Phlebology. DOI: 10.1177/02683555221145779




