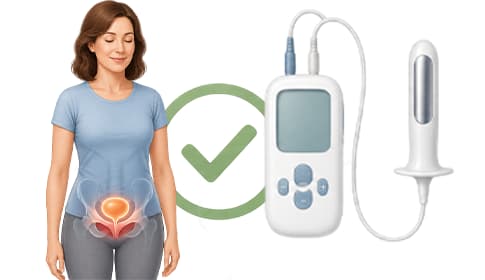
What is incontinence?
What is incontinence?
Incontinence is not a disease, but a symptom. It is usually caused by weakness of the pelvic floor muscles or disturbances in neurological control. If you treat the underlying cause, the symptom can improve.